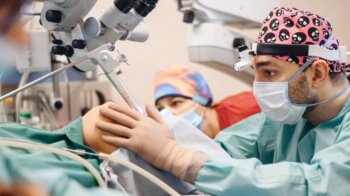
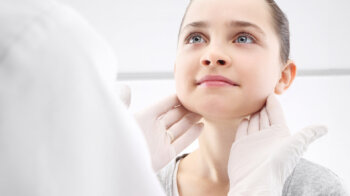
Its purpose is to improve nasal breathing in the patient. At the VIRTUS Institute of Advanced Medicine, this operation is performed using a laser, bipolar coagulator or cold plasma coblation method.
Unlike traumatic conchotomy and vasotomy, conchoplasty is a more modern method that involves only a careful reduction of the inferior turbinates, without affecting the middle and superior turbinates and other structures.
The main indication for conchoplasty is vasomotor rhinitis – pathological enlargement of the turbinates or hypertrophy of the turbinate mucosa. Vasomotor rhinitis is manifested by the following symptoms:
- nasal congestion;
- sneezing;
- difficulty in nasal breathing;
- copious clear discharge;
- frequent nosebleeds due to nasal congestion;
- constant dryness in the nose with or without the formation of crusts on the mucous membrane;
- nasal congestion in a horizontal position;
- congestion of the right/left half of the nose, lying on the right/left side, respectively;
- sensation of dripping down the back of the throat.
The main causes of vasomotor rhinitis are a deviated nasal septum and long-term use of vasoconstrictor drops.
In the first case, when a person has a deviated septum, the turbinates on the side of the narrowed nasal passage cannot expand when inhaling. This leads to disruption of the process of insulation, humidification and purification of incoming air, which is the main function of the nasal concha. Consequently, compensatoryly, on the side where there is expansion of the nasal sinus, the turbinates will expand more than usual. This will lead to their hypertrophy.
Therefore, when there is a deviated nasal septum, patients are often given a second diagnosis – vasomotor rhinitis. In this case, surgery to straighten a deviated septum (septoplasty) is not enough. Conchoplasty (if the curvature of the septum is minor) or septoconchoplasty (if the curvature is significant) is prescribed. Septoconchoplasty is a surgical procedure that straightens a deviated septum and reduces the inferior turbinates on one or both sides.
The second cause of vasomotor rhinitis in the form of long-term use of vasoconstrictor drops is associated with the specific anatomical structure of the nasal turbinates. They consist of cavernous (spongy) tissue with a large accumulation of vessels represented by muscle tissue. The latter must constantly work – contract and relax.
With the development of a runny nose, the blood vessels relax, swelling, inflammation, congestion and rhinorrhea form. When using the drops, an artificial contraction of the muscles occurs, and the symptoms temporarily disappear. But the effect is not long lasting. To prolong it, with each episode of congestion the person uses the drops again. Frequent and long-term use of vasoconstrictors leads to the fact that without them, the muscles are in a constantly relaxed state and cease to contract back on their own. As a result, hypertrophy of the nasal mucosa develops, associated with the use of vasoconstrictor drops, which is also called drug-induced rhinitis.
The maximum time for taking vasoconstrictor drops for both children and adults is 5-7 days. They are strictly prohibited for pregnant women, and if taken for a long time, they can cause headaches, migraines, ischemic stroke, nosebleeds and other complications.
Indications and contraindications for conchoplasty
The main indication for surgery is hypertrophy of the nasal turbinate mucosa. However, hypertrophy of the nasal sinuses is not a reason for surgical intervention. This is an expansion of the nasal passage, which most often does not lead to pathological conditions. Indications for conchoplasty are also:
- enlargement of the inferior turbinates;
- chronic vasomotor rhinitis;
- violation of nasal breathing;
- dependence on vasoconstrictors.
Conchoplasty is contraindicated:
- diseases of the blood coagulation system;
- neoplasms in the nasal concha (hemangiomas).
There may also be temporary contraindications to surgery for chronic hypertrophic rhinitis: acute infectious pathologies, some systemic diseases, pregnancy and lactation.
For children under 18 years of age, conchoplasty is performed only for direct indications.
The result of conchoplasty
The result of surgery for vasomotor rhinitis is correct nasal breathing without vasoconstrictor drugs. In addition, the functionality of the nasal turbinates is restored.
Rehabilitation after conchoplasty
The complete rehabilitation process after endoscopic conchoplasty takes 1 month.
The next day after the operation, the patient begins taking the medications prescribed and given to him. Within 5 days, his hemostatic sponge dissolves. An examination is scheduled for 5-7 days. During this procedure, the remnants of the hemostatic sponge are removed by suction.
Over the next time, the nasal mucosa begins to heal, becoming covered with a crust over the entire surface. Underneath, a healthy nasal mucosa slowly forms.
After conchoplasty, the following are prohibited for two weeks:
- intense physical activity;
- air travel;
- visiting the sauna, bathhouse and swimming pool.
Otherwise, severe bleeding may begin, which often has to be stopped with the help of a doctor.
Note that after surgery, the cavernous tissue may grow again over time. But this is only possible if the patient has a significant curvature of the nasal septum, but during conchoplasty, he was not ready for septoplasty, or the patient again begins to abuse vasoconstrictors.
What happens if vasomotor rhinitis is not treated?
If a person breathes poorly, but does not undergo conchoplasty, he will be dependent on vasoconstrictors or nasal congestion for life. In some situations, the breathing problem can get worse. For example, with the development of hypertension and weight gain.
















 207
207  1 min.
1 min.